MODULE eleven short answer questions.
saq 1.
A 45 year old man presents to the emergency department after having been intubated by the retrieval service. He has poured petrol over himself and self immolated. On examination the patient has full thickness burns to the entire chest and abdomen, his entire back and circumferential burns to both upper limbs and head. You estimate a weight of 80kg.
Question 1. (2 marks)
What percentage of body surface area has been burnt? Give the underlying basis for your answer.
Must include:
-Rule of 9’s
-Estimate BSA affected as 63% using the rule of 9s (9% each arm, 18% each front and back of torso, and 9% head.
Question 2. (1 mark)
Is there a more accurate way to assess BSA than your estimate above?
Must include:
-yes: a Lund and Browder chart.
Question 3. (3 marks)
What fluid regime will you prescribe for this patient?
Must include (1 mark for calculation, 1 mark for timings, 1 mark for specifying Hartmann's):
-20.16L (20 is acceptable) of Hartmann’s solution: 10L in the first 8 hours and the other 10L over 16 hours
[Note the underlying basis is the Parkland formula:
Parkland formula: fluid = %BSA x weight in kg x 4ml/kg
Half is given in the 1st 8 hours from the time of burn, the other half in the next 16 hours.]
Question 4. (2 marks)
Give two ways will you assess the accuracy of your fluid resuscitation.
Must include:
-IDC for urine output aim 1ml/kg.hr
Plus either:
-lactate clearance >50% over 4 hours (or something similar)
-serial renal function tests
Question 5. (1 mark)
The patient is intubated shortly after you commence your fluid resuscitation.
Post intubation you note oxygen saturations of 85%, tidal volumes of 300ml and peak airway pressures of 40cm H2O despite ventilation of 500ml SIMV and 100% O2.
What action will you now take?
Must include thoracic escharotomy
Question 6. (6 marks)
Describe the procedure you will perform.
Must include:
-procedure - diathermy pencil, set to coag at 20mV or scalpel (1 mark)
-chlorhexidine wash if available (1 mark)
-cut anterior axillary lines from clavicle to base of both iliac fossae. (1 marks)
-join over pubic margin, costal margin and collarbones (1 marks)
-final cut down sternum (1 marks)
-depth: through eschar down to subcutaneous fat (1 marks)
Question 1. (2 marks)
What percentage of body surface area has been burnt? Give the underlying basis for your answer.
Must include:
-Rule of 9’s
-Estimate BSA affected as 63% using the rule of 9s (9% each arm, 18% each front and back of torso, and 9% head.
Question 2. (1 mark)
Is there a more accurate way to assess BSA than your estimate above?
Must include:
-yes: a Lund and Browder chart.
Question 3. (3 marks)
What fluid regime will you prescribe for this patient?
Must include (1 mark for calculation, 1 mark for timings, 1 mark for specifying Hartmann's):
-20.16L (20 is acceptable) of Hartmann’s solution: 10L in the first 8 hours and the other 10L over 16 hours
[Note the underlying basis is the Parkland formula:
Parkland formula: fluid = %BSA x weight in kg x 4ml/kg
Half is given in the 1st 8 hours from the time of burn, the other half in the next 16 hours.]
Question 4. (2 marks)
Give two ways will you assess the accuracy of your fluid resuscitation.
Must include:
-IDC for urine output aim 1ml/kg.hr
Plus either:
-lactate clearance >50% over 4 hours (or something similar)
-serial renal function tests
Question 5. (1 mark)
The patient is intubated shortly after you commence your fluid resuscitation.
Post intubation you note oxygen saturations of 85%, tidal volumes of 300ml and peak airway pressures of 40cm H2O despite ventilation of 500ml SIMV and 100% O2.
What action will you now take?
Must include thoracic escharotomy
Question 6. (6 marks)
Describe the procedure you will perform.
Must include:
-procedure - diathermy pencil, set to coag at 20mV or scalpel (1 mark)
-chlorhexidine wash if available (1 mark)
-cut anterior axillary lines from clavicle to base of both iliac fossae. (1 marks)
-join over pubic margin, costal margin and collarbones (1 marks)
-final cut down sternum (1 marks)
-depth: through eschar down to subcutaneous fat (1 marks)
saq 2.
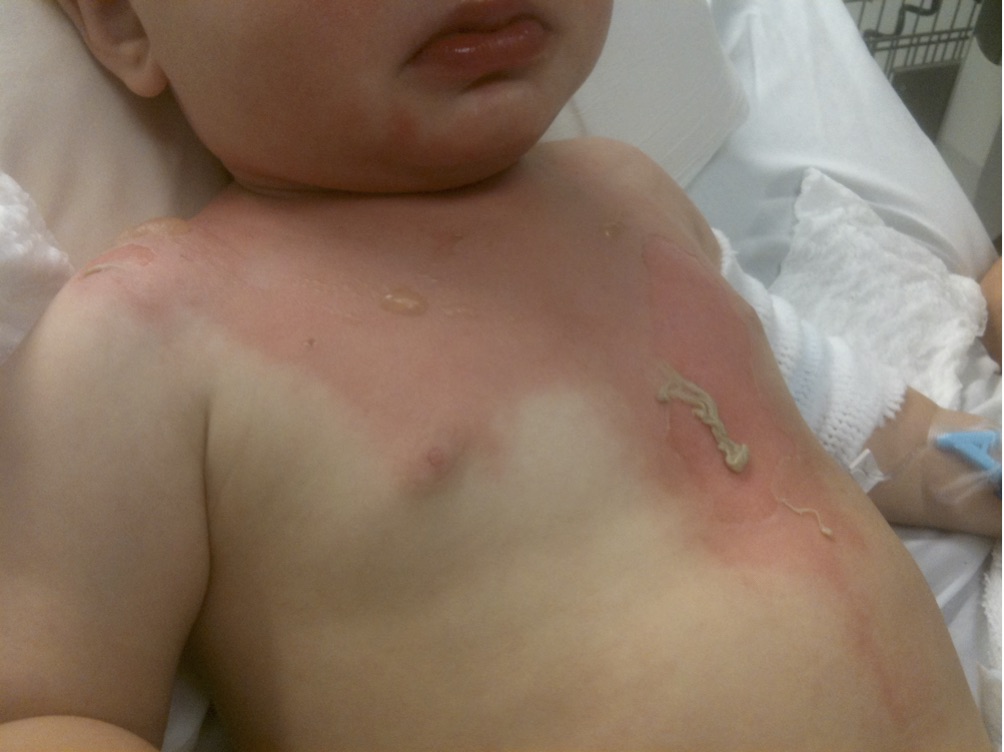
A 2 year old child presents to the ED with his mother after pulling a bowl of hot noodles down onto himself. A clinical image of the child is shown below.
Question 1. (2 marks)
Give 2 important features of the photo.
Must include:
-large area of erythema extending from neck to nipple line
-several blisters and skin sloughing over L nipple
Question 2. (1 mark)
What are the likely depth of these burns?
Must include:
-superficial to superficial partial thickness
Question 3. (3 marks)
Give 3 important steps in your initial management.
Must include:
-strong analgesia: 2 mcg/kg intranasal fentanyl or similar (as child has an IV will also accept intravenous reasonable intravenous analgesia eg morphine 0.1mg/kg as an answer)
Plus any of:
-check tetanus status and update as required
-clean wounds and remove devitalized tissue as able
-dress appropriately: Ag impregnated dressing or cream such as MepilexAg or Flamazine
-discussion with paediatric burns service to arrange follow up
Question 4. (4 marks)
Fill in the following table to indicate the type of tetanus prophylaxis required for immunized and non immunized patients who receive tetanus prone wounds.
Give 2 important features of the photo.
Must include:
-large area of erythema extending from neck to nipple line
-several blisters and skin sloughing over L nipple
Question 2. (1 mark)
What are the likely depth of these burns?
Must include:
-superficial to superficial partial thickness
Question 3. (3 marks)
Give 3 important steps in your initial management.
Must include:
-strong analgesia: 2 mcg/kg intranasal fentanyl or similar (as child has an IV will also accept intravenous reasonable intravenous analgesia eg morphine 0.1mg/kg as an answer)
Plus any of:
-check tetanus status and update as required
-clean wounds and remove devitalized tissue as able
-dress appropriately: Ag impregnated dressing or cream such as MepilexAg or Flamazine
-discussion with paediatric burns service to arrange follow up
Question 4. (4 marks)
Fill in the following table to indicate the type of tetanus prophylaxis required for immunized and non immunized patients who receive tetanus prone wounds.
|
TETANUS RISK
LOW HIGH |
UNIMMUNIZED
Give ADT in ED and refer for a full course of immunization Give ADT, refer for full course of immunization and administer 250IU IM tetanus IG |
IMMUNIZED
give ADT if time to last tetanus exceeds 10 years give ADT if time to last tetanus exceeds 5 years |
saq 3.
A 45 year old electrician presents to the emergency department after receiving an electric shock at work from a 240V AC mains outlet. He touched an extension cord that had exposed wire, and received a shock which jolted him backwards.
Question 1. (3 marks)
Give three features will you look for on examination?
Must include:
Assessment of any burns to hand which touched cord
Plus any of:
derangement of vital signs
secondary injury (head, orthopaedic etc)
neurological/cognitive impairment.
Question 2. (2 marks)
The patient subsequently has a normal physical examination. Which investigation will you perform and why?
Must include:
ECG: check evidence of cardiac injury or conduction defect
Question 3. (5 marks)
Fill in the following table for patterns of injury associated with electrical injury.
Question 1. (3 marks)
Give three features will you look for on examination?
Must include:
Assessment of any burns to hand which touched cord
Plus any of:
derangement of vital signs
secondary injury (head, orthopaedic etc)
neurological/cognitive impairment.
Question 2. (2 marks)
The patient subsequently has a normal physical examination. Which investigation will you perform and why?
Must include:
ECG: check evidence of cardiac injury or conduction defect
Question 3. (5 marks)
Fill in the following table for patterns of injury associated with electrical injury.
|
VOLTAGE
Low (<1000 volts) High (>1000 volts) Lightning Strike |
EXAMPLE OF EXPOSURE
240V AC mains outlet Downed power lines Industrial power sources (eg work site generator) N/A |
PATTERNS OF INJURY
Energy largely expended at site of contact - presents with deep cutaneous burns, often extensive tissue necrosis underneath skin Large internal current -deep compartment necrosis requiring fasciotomy - cardiac arrest if crosses chest Lichtenburg figures keraunoparalysis blunt/concussive trauma |
saq 4.
A 75 year old woman presents after falling on her outstretched right arm. She is right hand dominant and normally lives independently. The arm is significantly deformed, but she has no other injuries. Her medical history includes a NSTEMI 6 months prior, as well as COPD which limits her exercise tolerance to 100m.
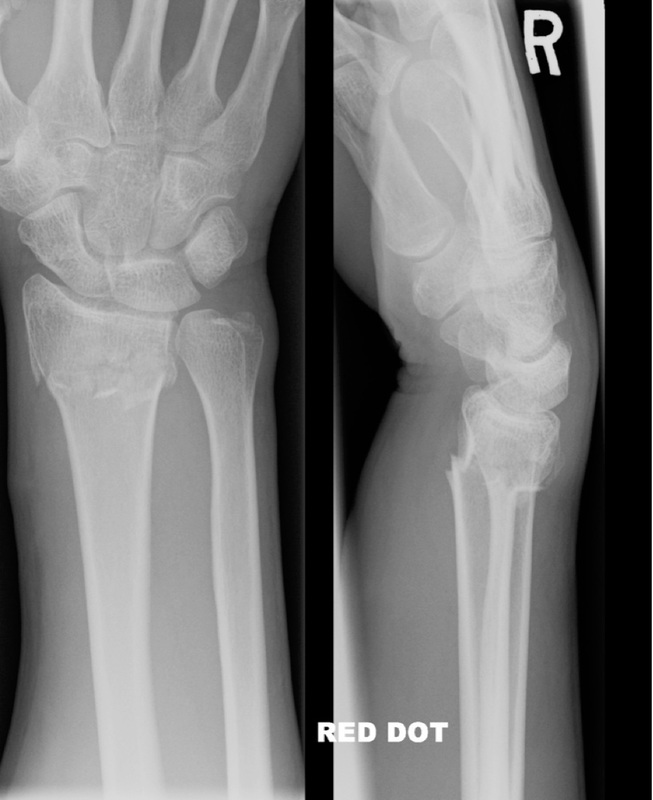
Plain radiographs of the forearm are shown below.
Plain radiographs of the forearm are shown below.
Question 1. (2 marks)
Describe 2 major findings on the xray.
Must include (1 mark each)
impacted, comminuted distal radius fracture
dorsal angulation (ie a Colles fracture.)
Question 2. (2 marks)
Your registrar asks you to provide sedation so that the fracture can be reduced in ED. What is your response?
Must include:
-this patient is ASA 3, and not suitable for ED procedural sedation.
Question 3. (8 marks)
Discuss four safe management strategies for this patient’s fracture using the format below.
Must include any 4 of the following
Describe 2 major findings on the xray.
Must include (1 mark each)
impacted, comminuted distal radius fracture
dorsal angulation (ie a Colles fracture.)
Question 2. (2 marks)
Your registrar asks you to provide sedation so that the fracture can be reduced in ED. What is your response?
Must include:
-this patient is ASA 3, and not suitable for ED procedural sedation.
Question 3. (8 marks)
Discuss four safe management strategies for this patient’s fracture using the format below.
Must include any 4 of the following
|
STRATEGY
1. Non reduction/conservative Mx 2. Haematoma block 3. Bier’s block 4. Reduction in OT 5. Brachial plexus block |
PRO
No anaesthetic required No anaesthetic required, can be done in ED Done in ED, lower risk than general anaesthesia Can use image intensification, anaesthetist can provide anaesthesia No anaesthetic required |
CON
dominant hand, suboptimal position risk of infection, variable efficacy labour intensive, risk of local anaesthetic toxicity, requires BP <150mmHg resource intensive, may be delay to treatment Technically complex |
NOTE, as this patient is ASA 3, procedural sedation is NOT considered a safe management strategy in the ED and scores NO marks.
SAQ 5.
A 31 year old male is brought in by the ambulance after being struck by a car whilst crossing the street. Bystanders report that the car struck him directly in the waist.
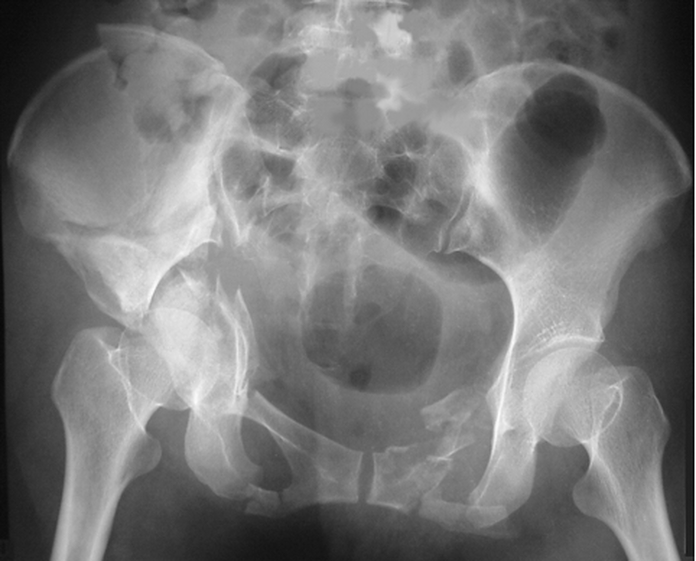
A trauma xray is shown below.
A trauma xray is shown below.
Question 1 (4 marks).
Give 4 major abnormalities seen on the xray.
Must include:
-no pelvic binder applied!
-comminuted fracture of the inferior and superior pubic rami bilaterally
-comminuted right acetabular fracture
-fracture of the left iliac wing
Question 2. (3 marks)
What features on clinical examination will make you suspect a urethral injury?
Must include:
-blood at external urethral meatus
-high riding prostate on PR exam
-scrotal haematoma
Question 3. (3 marks)
After CT "pan scanning" no other injuries are identified. After 4 units of blood the patient's blood pressure is 92/60mmHg and his HR is 114/min. The orthopaedic registrar has some doubt over the disposition of this patient. What will you tell her?
Must include:
-this is an unstable patient who needs definitive control of his haemorrhage (1 mark)
-for this injury the management is external fixation of the pelvis with either a binder or X-FIX, and internal packing against this fixation. (2 marks)
Give 4 major abnormalities seen on the xray.
Must include:
-no pelvic binder applied!
-comminuted fracture of the inferior and superior pubic rami bilaterally
-comminuted right acetabular fracture
-fracture of the left iliac wing
Question 2. (3 marks)
What features on clinical examination will make you suspect a urethral injury?
Must include:
-blood at external urethral meatus
-high riding prostate on PR exam
-scrotal haematoma
Question 3. (3 marks)
After CT "pan scanning" no other injuries are identified. After 4 units of blood the patient's blood pressure is 92/60mmHg and his HR is 114/min. The orthopaedic registrar has some doubt over the disposition of this patient. What will you tell her?
Must include:
-this is an unstable patient who needs definitive control of his haemorrhage (1 mark)
-for this injury the management is external fixation of the pelvis with either a binder or X-FIX, and internal packing against this fixation. (2 marks)
SAQ 6 to get the details please read the blog on resus.com.au Pregnancy and trauma
A 32 year old woman who is 24 weeks pregnant is brought into the emergency department by ambulance. She was a passenger in a high speed motor vehicle accident. She has no other relevant past history.
She has sustained a head injury with an episode of loss of consciousness. She has a small scalp laceration and has right lateral chest wall tenderness to palpation.
1. Complete below indicating which parameter increases or decreases in pregnancy
Maternal Heart rate: increases
Maternal Blood volume: increases
Maternal white cell count: increases
Maternal CO2: decreases
Maternal Functional residual capacity: decreases
Maternal rate of gastric emptying: decreases
2. You decide to perform an eFAST examination. The abdomen looks normal, however you are concerned about a potential pneumothorax on ultrasound. You speak to the patient about performing a CXR to look for a pneumothorax. The patient is concerned about radiation exposure of the fetus.
(a) What is considered a safe level of exposure during pregnancy? < 5 rads
(b) What is the exposure of a:
i.CXR? 0.005 rad
ii.Pelvic XRay? 0.4 rad
iii.CT Brain? 0.5 rad
iv.CT abdomen? 3.5 rad
3 You perform a CXR which shows a large right sided pneumothorax and 3 fractured ribs. You decide to insert a chest tube. Please briefly outline the position of insertion of the tube as it relates to the obstetric patient.
If a chest tube is needed aim to insert 1-2 intercostal spaces higher
4 You decide to monitor with cardiotocography
(a) How long should you monitor a patient for?
This is a controversial area. It is agreed that a minimum of 4 hours of CTG monitoring is needed. This may be sufficient for minor trauma such as falls, where it has been found that at 4 hours, if uterine contractions have ceased, especially after minor injury then the patient can be taken off monitoring. For more significant trauma, 24 – 48 hours of monitoring is needed.
(b) List the specific information you are looking
-List one thing you are looking for in the mother
-List 3 things you look for in terms of the fetal heart rate
CTG monitoring gives us information on:
5 List 3 ways in which placental abruption can present.
Uterine pain
Vaginal bleeding
Pre-term labour
She has sustained a head injury with an episode of loss of consciousness. She has a small scalp laceration and has right lateral chest wall tenderness to palpation.
1. Complete below indicating which parameter increases or decreases in pregnancy
Maternal Heart rate: increases
Maternal Blood volume: increases
Maternal white cell count: increases
Maternal CO2: decreases
Maternal Functional residual capacity: decreases
Maternal rate of gastric emptying: decreases
2. You decide to perform an eFAST examination. The abdomen looks normal, however you are concerned about a potential pneumothorax on ultrasound. You speak to the patient about performing a CXR to look for a pneumothorax. The patient is concerned about radiation exposure of the fetus.
(a) What is considered a safe level of exposure during pregnancy? < 5 rads
(b) What is the exposure of a:
i.CXR? 0.005 rad
ii.Pelvic XRay? 0.4 rad
iii.CT Brain? 0.5 rad
iv.CT abdomen? 3.5 rad
3 You perform a CXR which shows a large right sided pneumothorax and 3 fractured ribs. You decide to insert a chest tube. Please briefly outline the position of insertion of the tube as it relates to the obstetric patient.
If a chest tube is needed aim to insert 1-2 intercostal spaces higher
- The diaphragm rises by approximately 4cm
- The chest diameter increases
- This all results in an increased substernal angle
4 You decide to monitor with cardiotocography
(a) How long should you monitor a patient for?
This is a controversial area. It is agreed that a minimum of 4 hours of CTG monitoring is needed. This may be sufficient for minor trauma such as falls, where it has been found that at 4 hours, if uterine contractions have ceased, especially after minor injury then the patient can be taken off monitoring. For more significant trauma, 24 – 48 hours of monitoring is needed.
(b) List the specific information you are looking
-List one thing you are looking for in the mother
-List 3 things you look for in terms of the fetal heart rate
CTG monitoring gives us information on:
- Uterine Activity(contractions)
- These are a common finding, occurring in about 40% of trauma cases. Most resolve with no adverse fetal effects.
- The basal uterine tone and the frequency and intensity of contractions is important
- Fetal Heart Rate
- Compromised fetal perfusion and oxygenation presents with abnormal fetal heart rate
- The absolute rate is important ie both bradycardia or tachycardias
- Deceleration patterns are also important as is
- Loss of variability.
5 List 3 ways in which placental abruption can present.
Uterine pain
Vaginal bleeding
Pre-term labour