MODULE 17 short answer questions.
saq 1.
A 45 year old man presents to your department with pleuritic chest pain.
Question 1. (9 marks)
List the components of the PERC score you will consider in assessing this man.
Must include:
Age ≥ 50
HR ≥ 100
O2 Sat on Room Air < 95%
Prior History of Venous Thromboembolism
Trauma or Surgery within 4 weeks
Hemoptysis
Exogenous Estrogen
Unilateral Leg Swelling
And the opinion of an experienced clinician that a PE is “unlikely”.
Question 2. (6 marks)
Explain the difference between the PERC score and the Well’s score.
Must include:
PERC is used to assess risk of PE: – if –ve the NPV is >99% and no tests need to be performed. (2 marks)
Wells’ describes a pretest probability and can be used as a two or three tiered test. (2 marks)
In the two tiered test a score less than 4 indicates low risk and allows a screening test of sufficient sensitivity (a d-dimer) to be used with >99% NPV. (2 marks)
Question 1. (9 marks)
List the components of the PERC score you will consider in assessing this man.
Must include:
Age ≥ 50
HR ≥ 100
O2 Sat on Room Air < 95%
Prior History of Venous Thromboembolism
Trauma or Surgery within 4 weeks
Hemoptysis
Exogenous Estrogen
Unilateral Leg Swelling
And the opinion of an experienced clinician that a PE is “unlikely”.
Question 2. (6 marks)
Explain the difference between the PERC score and the Well’s score.
Must include:
PERC is used to assess risk of PE: – if –ve the NPV is >99% and no tests need to be performed. (2 marks)
Wells’ describes a pretest probability and can be used as a two or three tiered test. (2 marks)
In the two tiered test a score less than 4 indicates low risk and allows a screening test of sufficient sensitivity (a d-dimer) to be used with >99% NPV. (2 marks)
saq 2.
Using the table below compare and contrast CTPA, V/Q scan and echocardiography for the investigation of suspected PE.
|
Diagnostic yield Diagnostic issues Side effects |
CTPA
|
V/Q scan
|
Echocardiogram
|
saq 3.
A 66 year old female with a history of COAD presents to your emergency department with increasing dyspnoea. Her vital signs are:
HR 105 /min
BP 115/62 mmHg
RR 32 /min
Sats 88% 6L
T 37.9 oC
Question 1. (7 marks)
A venous blood gas is taken urgently in the resus room and the results are shown below.
FiO2 0.5
pH 7.12
pO2 43 mmHg
pCO2 78 mmHg
HCO3 25 mmol/L
BE -5
Na+ 141 mmol/L
K+ 6.5 mmol/L
Cl- 99 mmol/L
Lactate 4.1 mmol/L
Give the major acid base disturbances present and justify your answer. Include a likely unifying diagnosis.
Must include:
Respiratory acidosis (1 mark)
Expect HCO3- acutely = 28 or chronically to = 40. (2 marks)
CO2 is only 25! .: diagnose a metabolic acidosis and concurrent metabolic alkalosis (2 marks)
This is likely due to chronic CO2 retention, and an acute infective exacerbation of COPD with sepsis. (2 marks)
Question 2. (5 marks)
Give 5 interventions you will immediately apply.
Must include:
Question 3. (4 marks)
Give 4 instances in which you will discontinue your respiratory support in this patient.
Must include:
(Or other reasonable statements - feel free to post up on the VSG for discussion.)
HR 105 /min
BP 115/62 mmHg
RR 32 /min
Sats 88% 6L
T 37.9 oC
Question 1. (7 marks)
A venous blood gas is taken urgently in the resus room and the results are shown below.
FiO2 0.5
pH 7.12
pO2 43 mmHg
pCO2 78 mmHg
HCO3 25 mmol/L
BE -5
Na+ 141 mmol/L
K+ 6.5 mmol/L
Cl- 99 mmol/L
Lactate 4.1 mmol/L
Give the major acid base disturbances present and justify your answer. Include a likely unifying diagnosis.
Must include:
Respiratory acidosis (1 mark)
Expect HCO3- acutely = 28 or chronically to = 40. (2 marks)
CO2 is only 25! .: diagnose a metabolic acidosis and concurrent metabolic alkalosis (2 marks)
This is likely due to chronic CO2 retention, and an acute infective exacerbation of COPD with sepsis. (2 marks)
Question 2. (5 marks)
Give 5 interventions you will immediately apply.
Must include:
- Start Bi-level non invasive ventilation 10/5 cmH20 (or similar settings)
- Supplemental oxygen for sats >90%
- Administer nebulized salbutamol 5mg and ipratropium 500mcg
- IV hydrocortisone 200mg
- Appropriate antibiotics and dose: eg penicillin plus a macrolide (ampicillin 1g IV and azithromycin 500mg IV)
Question 3. (4 marks)
Give 4 instances in which you will discontinue your respiratory support in this patient.
Must include:
- Patient deteriorates and requires intubation/CPR
- Patient vomits or loses airway
- Respiratory acidosis resolves
- Patient cannot tolerate BiPAP
(Or other reasonable statements - feel free to post up on the VSG for discussion.)
saq 4.
A 45 year old patient presents to your department in tropical Australia complaining of a fever and productive cough. He has a history of poorly controlled type II diabetes and excess alcohol use.
His vital signs are:
HR 125 /min
BP 95/55 mmHg
RR 35 /min
Sats 91% 4L
T 39.9 oC
Question 1. (6 marks)
List three atypical organisms/disease you will consider in this patient’s presentation, and how you will specifically investigate for each.
Must include:
- Burkholderia Pseudomallei/Meliodosis: blood cultures with ashdown’s agar (only 0.5 marks if BCs are specified without the specific medium or request)
- Coxiella Burnetti/Q Fever: PCR
Plus any other reasonable combination such as:
TB – Z/N stain
Scrub typhus – rickettsial serology
Lyme disease – same
Dengue Fever – arboviral serology
Etc. (Feel free to post your answers via the VSG!)
Question 2. (3 marks)
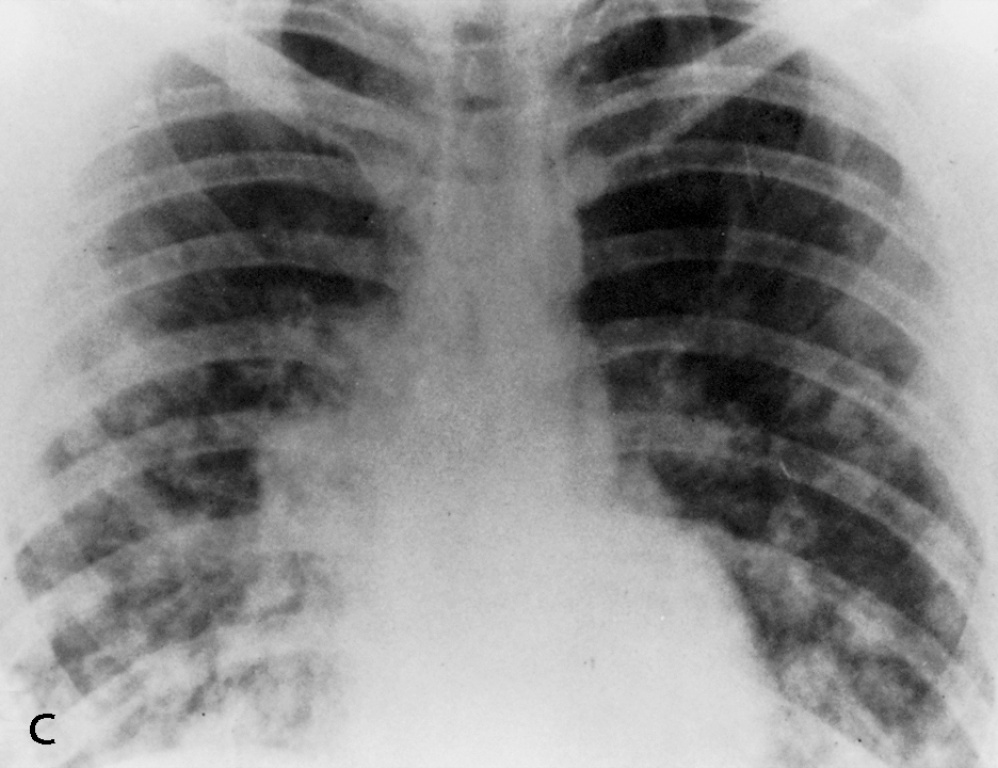
The patient’s chest xray is shown below. What are the main features and which diagnosis do they suggest?
Must include:
Question 3. (2 marks)
What antibiotics will you treat this patient with?
Must include:
- Patchy bibasal infiltration/consolidation
- Very concerning for Meliodosis
Question 3. (2 marks)
What antibiotics will you treat this patient with?
Must include:
- Appropriate antibiotics for severe tropical CAP
- Meropenem 1g
- Azithromycin 500mg
SAQ 5.
A 22 year old female presents to your department complaining of acute dyspnoea. She is quite anxious and looks distressed.
Question 1. (5 marks)
List 5 indicators of life threatening asthma that you will assess this patient for.
Must include:
Question 2. (5 marks)
The patient has blue lips and an oxygen saturation of 89% on 2L of O2.
Give 5 interventions you will immediately undertake.
Must include:
Question 3.
The patient is not responding to your therapy above. What escalation of therapy will you implement.
Must include:
Question 4. (3 marks)
If the patient requires intubation, what principles will you use to set the ventilator?
Must include:
Question 1. (5 marks)
List 5 indicators of life threatening asthma that you will assess this patient for.
Must include:
- Reduced consciousness or collapse
- Exhaustion
- Cyanosis
- Oxygen saturation <90%
- Reduced or absent breath sounds
Question 2. (5 marks)
The patient has blue lips and an oxygen saturation of 89% on 2L of O2.
Give 5 interventions you will immediately undertake.
Must include:
- High flow supplemental oxygen for sats >95%
- Continuous nebulized salbutamol
- 3x nebulized iptratropium 500mcg
- IV hydrocortisone 200mg
- IV MgSO4 20mmol
Question 3.
The patient is not responding to your therapy above. What escalation of therapy will you implement.
Must include:
- Either salbutamol infusion titrated from 5mcg/kg per hour or adrenaline infusion similarly
Question 4. (3 marks)
If the patient requires intubation, what principles will you use to set the ventilator?
Must include:
- Low i:e ratio (eg 1:4)
- High FiO2, aiming for normoxia with permissive hypocapnoea
- Ideally minimise airway pressures