MODULE FOUR short answer questions.
saq 1.
SAQ 1.
A 72 year old man presents to the emergency department with brisk bleeding from the right nostril. He is applying pressure at the bridge (superior junction of the nose and face) of his nose without any improvement in the bleeding. He is warfarinized for atrial fibrillation, but otherwise has no medical history. He has no airway compromise, and his vital signs are:
HR 90 /min
BP 135/82 mmHg
RR 16 /min
Sats 99% RA
Temp 37.2 oC
A 72 year old man presents to the emergency department with brisk bleeding from the right nostril. He is applying pressure at the bridge (superior junction of the nose and face) of his nose without any improvement in the bleeding. He is warfarinized for atrial fibrillation, but otherwise has no medical history. He has no airway compromise, and his vital signs are:
HR 90 /min
BP 135/82 mmHg
RR 16 /min
Sats 99% RA
Temp 37.2 oC
Question 1. Give one intervention you will immediately apply and one investigation you will undertake. (2 marks)
Must include:
- lean forwards and apply pressure along the whole line of the nose for 10-15 minutes
- check INR
Question 2. The patient’s bleeding does not settle with your initial management. What therapeutic actions will you take now? (6 marks)
Must include:
- some form of nasal packing (2 marks)
- nasal tampons, can be inserted bilaterally
- gauze
- balloon catheter
-rapid rhino
- appropriate adjunct therapy (1 mark each)
- use of vasoconstrictor local anaesthetic (co-phenylcaine spray)
- use of topical antibiotic lubricant (bacitracin)
- discussion with ENT surgeon RE administration of IV antibiotics
- referral to an ENT surgeon for follow up (1 mark)
A typical answer may include:
Ask patient to blow nose and remove all clots
If obvious bleeding point in Kiesselbach's Plexus can cauterise, otherwise (1 points)
Insert co-phenylcaine soaked pledget and ask patient to continue holding nose- applying pressure along whole length of nose(1 points)
Re-check in 5 minutes- if not resolved proceed to insert packing device i.e. mercer tampon or rapid rhino(explain process)(2 points)
Commence oral antibiotics- Flucloxacillin 250mg po qid- controversial (1 point)
If elderly and 2 packs admit, otherwise packs should be removed within 24 hours (1 point)
Question 3. The patient continues to have a significant ooze of blood from his nose after your interventions. His INR returns at 10.3. What actions will you take? (2 marks)
Must include:
- administration of IV vitamin K 10mg
- administration of prothrombin complex concentrate 25-50IU/kg OR FFP 20ml/kg.
Must include:
- lean forwards and apply pressure along the whole line of the nose for 10-15 minutes
- check INR
Question 2. The patient’s bleeding does not settle with your initial management. What therapeutic actions will you take now? (6 marks)
Must include:
- some form of nasal packing (2 marks)
- nasal tampons, can be inserted bilaterally
- gauze
- balloon catheter
-rapid rhino
- appropriate adjunct therapy (1 mark each)
- use of vasoconstrictor local anaesthetic (co-phenylcaine spray)
- use of topical antibiotic lubricant (bacitracin)
- discussion with ENT surgeon RE administration of IV antibiotics
- referral to an ENT surgeon for follow up (1 mark)
A typical answer may include:
Ask patient to blow nose and remove all clots
If obvious bleeding point in Kiesselbach's Plexus can cauterise, otherwise (1 points)
Insert co-phenylcaine soaked pledget and ask patient to continue holding nose- applying pressure along whole length of nose(1 points)
Re-check in 5 minutes- if not resolved proceed to insert packing device i.e. mercer tampon or rapid rhino(explain process)(2 points)
Commence oral antibiotics- Flucloxacillin 250mg po qid- controversial (1 point)
If elderly and 2 packs admit, otherwise packs should be removed within 24 hours (1 point)
Question 3. The patient continues to have a significant ooze of blood from his nose after your interventions. His INR returns at 10.3. What actions will you take? (2 marks)
Must include:
- administration of IV vitamin K 10mg
- administration of prothrombin complex concentrate 25-50IU/kg OR FFP 20ml/kg.
saq 2.
A 38 year old injecting drug user presents complaining of dyspnoea and lassitude. He also has right sided neck pain.
His vital signs are:
HR 110 /min
BP 90/45 mmHg
RR 28 /min
Sats 99% RA
Temp 39.6 oC
Question 1. What specific features will you enquire about on history to assess this man’s airway? (3 marks)
Must include:
- voice changes
- ability to swallow own secretions
- presence of any obstructed flow noise (stridor/wheeze)
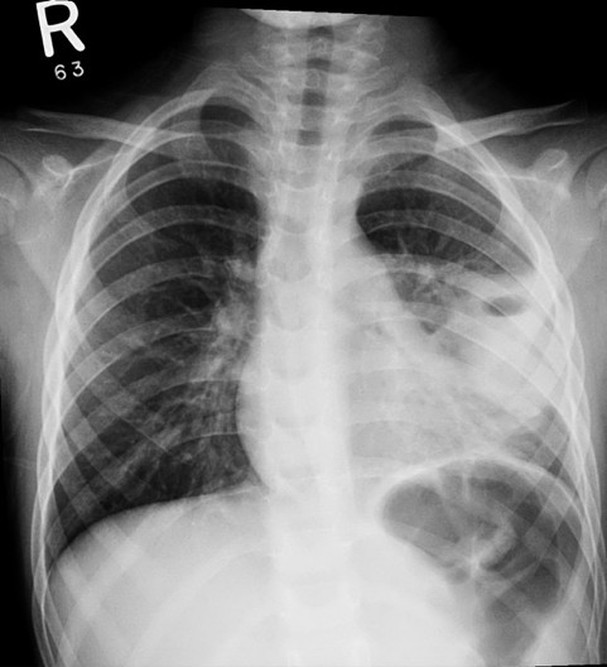
Question 2. A routine chest xray is performed, and is shown below. What does it show?(2 marks)
His vital signs are:
HR 110 /min
BP 90/45 mmHg
RR 28 /min
Sats 99% RA
Temp 39.6 oC
Question 1. What specific features will you enquire about on history to assess this man’s airway? (3 marks)
Must include:
- voice changes
- ability to swallow own secretions
- presence of any obstructed flow noise (stridor/wheeze)
Question 2. A routine chest xray is performed, and is shown below. What does it show?(2 marks)
Must include:
- left lower lobe consolidation
- air fluid level suggestive of lung abscess
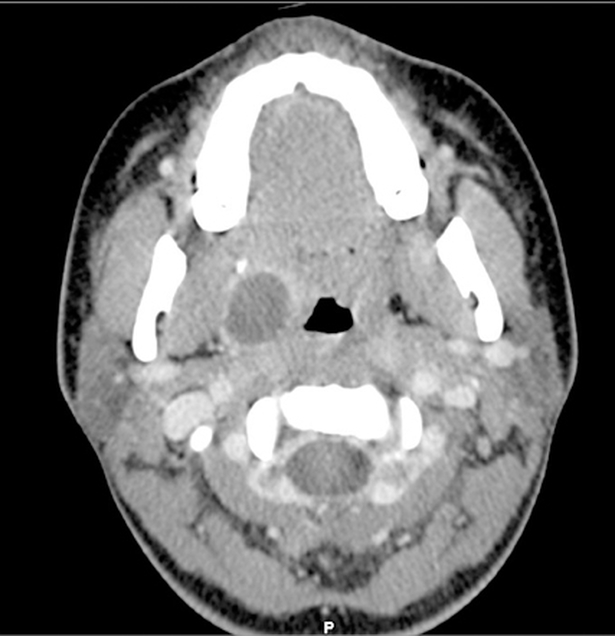
Question 3. The patient goes on to have a CT of the neck performed, and an image is shown below. Give 2 major abnormalities and the likely diagnosis. (3 marks)
- left lower lobe consolidation
- air fluid level suggestive of lung abscess
Question 3. The patient goes on to have a CT of the neck performed, and an image is shown below. Give 2 major abnormalities and the likely diagnosis. (3 marks)
Must include:
anterior thrombus in R internal jugular vein/dilation of right jugular vein
significant soft tissue abscess distorting normal airway anatomy
Diagnosis:
- septic thrombophlebitis of the internal jugular vein (Lemierre’s syndrome)
Question 4. Give 2 actions you will undertake to manage this patient. (2 marks)
Must include:
- administration of broad spectrum antibiotics - piperacillin/tazobactam 4.5g
- urgent referral to a head and neck surgeon
anterior thrombus in R internal jugular vein/dilation of right jugular vein
significant soft tissue abscess distorting normal airway anatomy
Diagnosis:
- septic thrombophlebitis of the internal jugular vein (Lemierre’s syndrome)
Question 4. Give 2 actions you will undertake to manage this patient. (2 marks)
Must include:
- administration of broad spectrum antibiotics - piperacillin/tazobactam 4.5g
- urgent referral to a head and neck surgeon
saq 3.
A 4 year old boy presents with his mother complaining of severe neck pain and an inability to turn the neck. His mother states he has been complaining of a sore throat for the past 3 days, but he has otherwise no medical history of note. On presentation he has visible drooling.
His vital signs are:
HR 125 /min
BP 91/66 /min
RR 38 /min
Sats 99% RA
T 39.1 oC
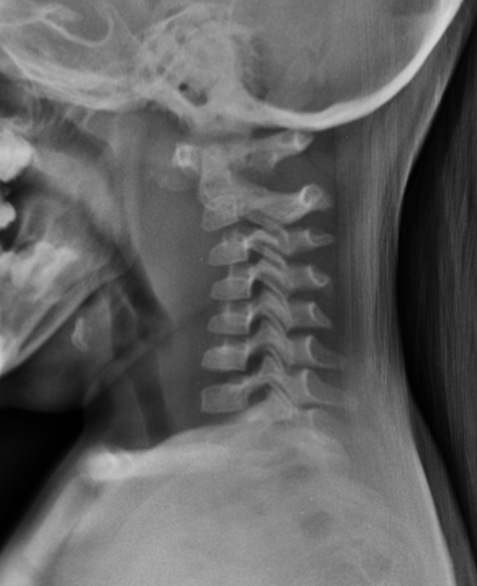
Your resident has ordered a plain film of the child’s neck which is shown below.
His vital signs are:
HR 125 /min
BP 91/66 /min
RR 38 /min
Sats 99% RA
T 39.1 oC
Your resident has ordered a plain film of the child’s neck which is shown below.
Question 1. What is the major abnormality and the likely diagnosis? (2 marks)
Must include:
- significant swelling of the prevertebral space/buccopharyngeal fascia anterior to C1-C4.
- suggests a retropharyngeal abscess
Question 2. Give four features you will examine for as part of you assessment of this child’s airway. (4 marks)
Must include:
- ability to swallow own secretions
- presence of stridor or wheeze
- posture - sitting forward, tripping
- work of breathing: tracheal tug or intercostal recession
Question 3. Give four management steps you will immediately undertake. (4 marks)
Must include:
- ampicillin (or equivalent) 50mg/kg IV stat
- analgesia: IN fentanyl 1.5ug/kg or IV analgesia (note, no marks for analgesia as stated patient is unable to swallow).
- urgent referral to an ENT surgeon for admission
saq 4.
A 19 year old female presents with a painful throat. She states she is unable to swallow food and water, and is feeling quite unwell. She also complains of difficulty in opening her mouth.
Her vital signs are:
HR 110 /min
BP 115/80mmHg
RR 20 /min
T 38.6 oC
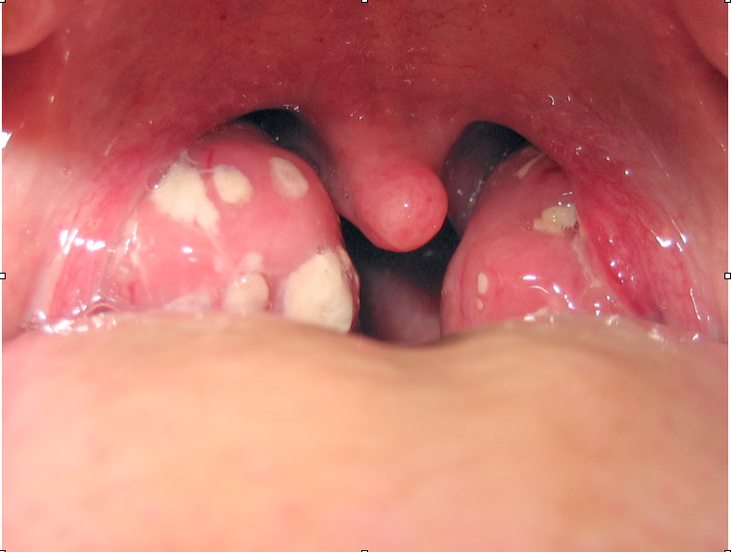
After analgesia you are able to examine the patient’s throat. A clinical image of the patient is shown below.
Question 1. Give three abnormalities and 2 differential diagnoses? (5 marks)
Her vital signs are:
HR 110 /min
BP 115/80mmHg
RR 20 /min
T 38.6 oC
After analgesia you are able to examine the patient’s throat. A clinical image of the patient is shown below.
Question 1. Give three abnormalities and 2 differential diagnoses? (5 marks)
Must include:
- bilaterally asymmetric swollen tonsils R>L
- large pustular exudates
- deviation of uvula to the left
Differential diagnoses (must include)
- Bacterial tonsillitis
- R peritonsillar abscess
Question 2. Give 5 management steps you will institute.
Must include:
- administration of high dose benzylpenicillin 1.2-2.4g IV QID
- analgesia: paracetamol 1g QID plus an adjunct
- dexamethasone 8mg IV
- IV fluid administration at a reasonable rate (eg 1L NaCl 0.9% over 4 - 8 hours)
- referral to an ENT surgeon for evaluation and drainage
- bilaterally asymmetric swollen tonsils R>L
- large pustular exudates
- deviation of uvula to the left
Differential diagnoses (must include)
- Bacterial tonsillitis
- R peritonsillar abscess
Question 2. Give 5 management steps you will institute.
Must include:
- administration of high dose benzylpenicillin 1.2-2.4g IV QID
- analgesia: paracetamol 1g QID plus an adjunct
- dexamethasone 8mg IV
- IV fluid administration at a reasonable rate (eg 1L NaCl 0.9% over 4 - 8 hours)
- referral to an ENT surgeon for evaluation and drainage
saq 5.
A 27 year old patient presents with a painful left ear. He has no medical history of note. He describes waking up to find green pus staining his pillow.
His vital signs are:
HR 79 /min
BP 120/78mmHg
RR 16 /min
T 37.6 oC
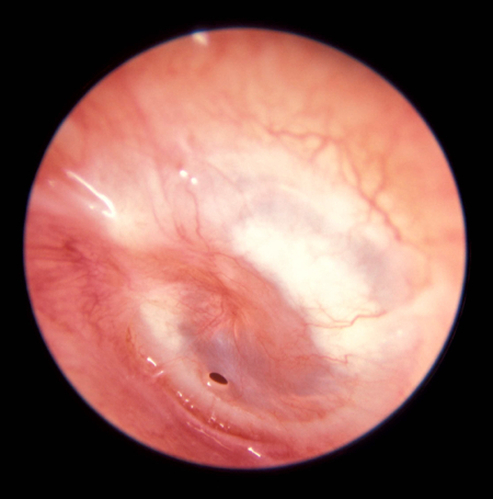
A clinical image of the patient’s examination findings is shown below.
His vital signs are:
HR 79 /min
BP 120/78mmHg
RR 16 /min
T 37.6 oC
A clinical image of the patient’s examination findings is shown below.
Question 1. Give 2 abnormalities and the diagnosis (3 marks)
Must include
- an inflamed tympanic membrane
- small perforation inferiorly
Diagnosis: acute otitis media (0.5 marks) complicated by perforation (0.5 marks)
Question 2. How will you manage this patient. (4 marks)
Must include:
- administration of oral antibiotics (amoxycillin 500mg tds or equivalent)
- analgesia: paracetamol 1g tds or ibuprofen 400mg tds
- advice to keep the ear dry/avoid swimming
- follow up with GP or ENT clinic within 2 weeks to ensure perforation has healed
Question 3. The patient returns to ED a week later, having not been compliant with the therapy you prescribed above. He is complaining of severe ear pain that extends behind his ear.
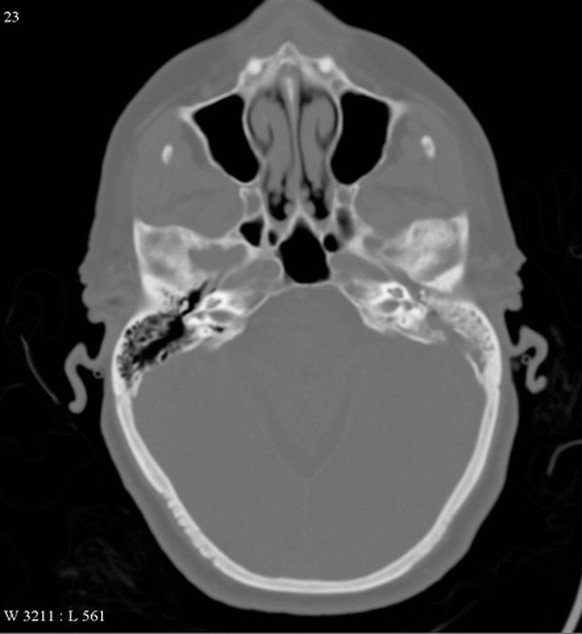
A CT scan of the patient’s head is performed. Give 2 abnormalities and the diagnosis. (3 marks)
Must include
- fluid in L mastoid air cells
- erosion of bone in mastoid air cells
Diagnosis: mastoiditis
Must include
- an inflamed tympanic membrane
- small perforation inferiorly
Diagnosis: acute otitis media (0.5 marks) complicated by perforation (0.5 marks)
Question 2. How will you manage this patient. (4 marks)
Must include:
- administration of oral antibiotics (amoxycillin 500mg tds or equivalent)
- analgesia: paracetamol 1g tds or ibuprofen 400mg tds
- advice to keep the ear dry/avoid swimming
- follow up with GP or ENT clinic within 2 weeks to ensure perforation has healed
Question 3. The patient returns to ED a week later, having not been compliant with the therapy you prescribed above. He is complaining of severe ear pain that extends behind his ear.
A CT scan of the patient’s head is performed. Give 2 abnormalities and the diagnosis. (3 marks)
Must include
- fluid in L mastoid air cells
- erosion of bone in mastoid air cells
Diagnosis: mastoiditis