Explanation
So, how did you find that? If you haven't actually made a bona fide attempt to answer the three questions STOP NOW, GO BACK AND GET A PIECE OF PAPER OUT. This particular question can be passed without reading the CT. (A total of 10 from 14 marks are possible in this fashion).
We're not advocating doing the exam without looking at the props of course. But hopefully the exercise we've just given you will illustrate our point: if you listen to what the examiners are saying it makes passing a whole lot easier.
*Listen* to what the examiners are telling you. Every exam, especially this one, has a language that allows examiners and examinees to communicate. Breaking down the questions and thinking about *why* and *how* you are being asked the questions is a big advantage compared to approaching them as a simple "write out some knowledge" type exercise.
We're not advocating doing the exam without looking at the props of course. But hopefully the exercise we've just given you will illustrate our point: if you listen to what the examiners are saying it makes passing a whole lot easier.
*Listen* to what the examiners are telling you. Every exam, especially this one, has a language that allows examiners and examinees to communicate. Breaking down the questions and thinking about *why* and *how* you are being asked the questions is a big advantage compared to approaching them as a simple "write out some knowledge" type exercise.
To remind you of our three questions:
If you read the clinical information carefully you would have noticed that this patient has had a severe headache, with a deterioration to GCS 11, hypertension and a normal temperature (so it's not meningitis!). The examiners have just told you the diagnosis.
Every question is about one problem and here it's highly likely that the patient has had a subarachnoid haemorrhage. Of course, a primary intraparenchymal haemorrhage is also a possibility, but typically severe headaches are used as a euphemism for SAH and that's what we're going to go with for the purpose of this exercise.
There's the answer to question 1 then done already.
We'll hypothesize that the CT shows a subarachnoid haemorrhage likely to be secondary to rupture of an aneurysm (possibly in the context of chronic hypertension). Of course, if we were actually looking at the CT we would specify a likely arterial territory (in the interests of writing as scientifically and definitively as possible, which was another point to take away from the face to face). BUT, for the purposes of the exercise you get the point.
Let's move on to question two.
Common radiological parameters used to assess severity include:
So, there's question two (half) answered. We'd need to actually see the CT to answer the other bits. (You could also name a few other poor CT prognostic features. Feel free to share some ideas on the VSG.)
Finally, we are asked for four prognostic factors in this patient. We have added the emphasis for a reason - in the examination report the examiners comment that people failed for listing general prognostic factors for subarachnoid haemorrhage, rather than listing those for this patient specifically.
We would answer question 4 with the following:
How do we actually do?
We score ourselves at 2/2 for question 1, 4/8 for question 2, and 3/4 for question 3.
All up that's 9/14: 64%.
Not bad, given we haven't looked at the major prop and therefore disqualified ourself from at least 4 marks.
Again, we're not advocating ripping up the prop booklets. But we would like you to think about the questions, and what the examiners are telling you.
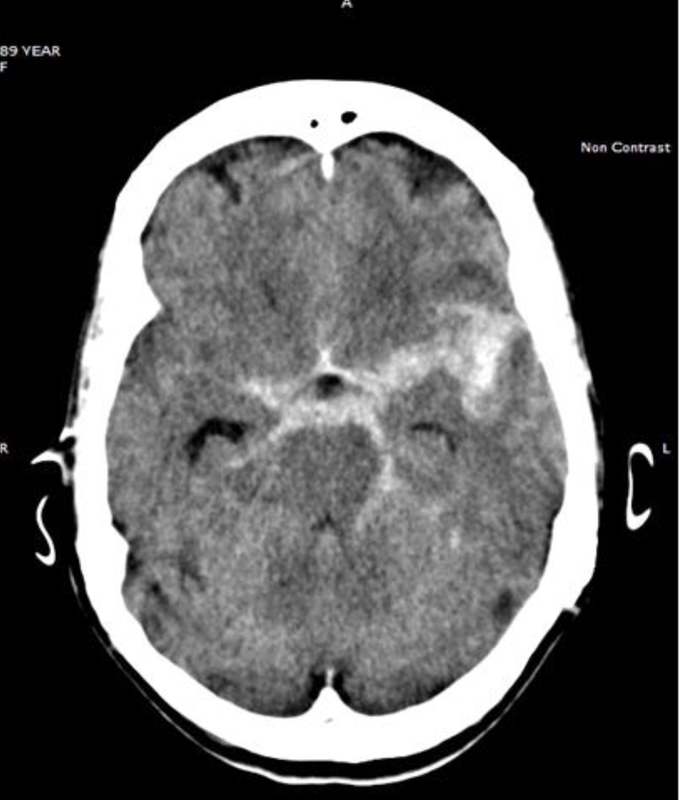
And for the record, the patient's CT is below.
- What is the abnormality on this patient's CT scan? (2 marks)
- What radiological parameters are used to indicate severity and are they present or absent? (8 marks)
- List four poor prognostic factors in this woman. (4 marks)
If you read the clinical information carefully you would have noticed that this patient has had a severe headache, with a deterioration to GCS 11, hypertension and a normal temperature (so it's not meningitis!). The examiners have just told you the diagnosis.
Every question is about one problem and here it's highly likely that the patient has had a subarachnoid haemorrhage. Of course, a primary intraparenchymal haemorrhage is also a possibility, but typically severe headaches are used as a euphemism for SAH and that's what we're going to go with for the purpose of this exercise.
There's the answer to question 1 then done already.
We'll hypothesize that the CT shows a subarachnoid haemorrhage likely to be secondary to rupture of an aneurysm (possibly in the context of chronic hypertension). Of course, if we were actually looking at the CT we would specify a likely arterial territory (in the interests of writing as scientifically and definitively as possible, which was another point to take away from the face to face). BUT, for the purposes of the exercise you get the point.
Let's move on to question two.
Common radiological parameters used to assess severity include:
- The degree of bleeding (as per the Fischer scale): intracerebral or ventricular blood is bad
- The presence of clots in the subarachnoid blood (the Fischer scale again)
- The presence of obstructive hydrocephalus
- Cerebral oedema: loss of the sulci/gyri and compression of the ventricles
So, there's question two (half) answered. We'd need to actually see the CT to answer the other bits. (You could also name a few other poor CT prognostic features. Feel free to share some ideas on the VSG.)
Finally, we are asked for four prognostic factors in this patient. We have added the emphasis for a reason - in the examination report the examiners comment that people failed for listing general prognostic factors for subarachnoid haemorrhage, rather than listing those for this patient specifically.
We would answer question 4 with the following:
- Advanced age (89)
- Altered level of consciousness (GCS 11)
- Large degree of intracerebral haemorrhage. (Note, we can't actually see the CT, but we've got a GCS 11 SAH. She's got to have a large bleed...)
- A fourth is a bit harder to come by without seeing the scan. If we had an extensive list of cormorbidities or anticoagulation we'd cite those, but we don't. In fact, we are specifically told the patient is otherwise well. So, it must be something else do with the CT scan - i.e. something that we've listed in question 2. If we had to, we'd either pick obstructive hydrocephalus or cerebral oedema as a 50:50 guess.
How do we actually do?
We score ourselves at 2/2 for question 1, 4/8 for question 2, and 3/4 for question 3.
All up that's 9/14: 64%.
Not bad, given we haven't looked at the major prop and therefore disqualified ourself from at least 4 marks.
Again, we're not advocating ripping up the prop booklets. But we would like you to think about the questions, and what the examiners are telling you.
And for the record, the patient's CT is below.