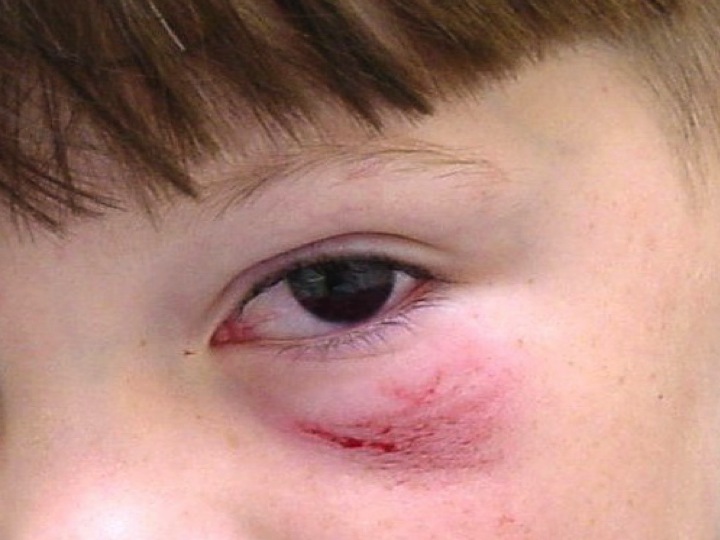
A 7 year old boy is brought to the emergency department by his teacher following an injury to the left eye that morning.
Describe and interpret the photo and outline your management.
Describe and interpret the photo and outline your management.
ANSWER & COMMENTARY
"Describe and interpret the photo and outline your management." Yes, that's really all we used to get in the old exam. It might sound a bit vague, but answering questions in this fashion is a good way to build clinical reasoning. The new examination aims to ask more specific questions, but really a candidate's thought process should not be too dissimilar in 2015 to that of a 2013 candidate.
The obvious findings on the photograph are a hyphaema of approx 30%. There is also a partial ptosis of the lid and infra-orbital abrasions.
However, in many ways this statements raises more questions than it asks. Every word in the examination question is important, and candidates should become proficient in formulating lists of major issues arising out of or suggested by the question stem. As examples see some of our thoughts below. Particularly candidates need to be able to talk about assessment (especially with regard to associated injuries and high risk features), immediate management priorities, and disposition considerations including "other" social (and often important) issues.
Being able to draw out these associations is a critical skill for candidates to develop in order to succeed in the fellowship examination.
1. A full assessment is needed.
We need to get a full history of how the injury occurred i.e.., what is the exact mechanism? We need to exclude other injuries, especially fractures of the orbit and globe rupture. Traumatic hyphaemas are usually the result of projectiles, however the abrasion may not fit in with this story. This is a grade 2 hyphaema ie., 1/3-1/2 of the pupil is obscured.
The history should include:
Examination should include:
Tonometry will also be needed as raised intraoccular pressure occurs in about 1/3 of cases. As a caveat if a globe rupture is suspected tonometry should not be performed as extra pressure may worsen extrusion of ocular contents. A globe rupture should be suspected with enopthalmos (intraoccqular content loss), exophthalmos due to retro-orbital haemorrhage, and a tear shaped or otherwise irregular pupil. Candidates should be prepared to mention the absence of these as important findings if required. Certainly the absence of an irregular pupil is an important negative finding in the photo above.
2. Most injuries require management
Management is a shield over the eye, rest, analgesia and sitting at a 30-45 degree angle to hasten clearing of the eye and improvement of visual acuity. An ophthalmologist should be quickly consulted by the emergency physician regarding this injury.
3. Disposition and social issues should always be considered.
Admission is indicated in this patient firstly because of the size of haematoma (certainly if there is any sickle cell trait) and secondly because there may be no-one available at home, which may be evidenced by the parents/carers not being present. Clued in candidates will also raise the issue as to why the parents are not present as the implication in the question is that this injury occurred earlier in the day (prior to school), and possibly represents non-accidental injury. Fellowship level candidates always do well to show perspective by consideration of NAI in paediatric presentations.
"Describe and interpret the photo and outline your management." Yes, that's really all we used to get in the old exam. It might sound a bit vague, but answering questions in this fashion is a good way to build clinical reasoning. The new examination aims to ask more specific questions, but really a candidate's thought process should not be too dissimilar in 2015 to that of a 2013 candidate.
The obvious findings on the photograph are a hyphaema of approx 30%. There is also a partial ptosis of the lid and infra-orbital abrasions.
However, in many ways this statements raises more questions than it asks. Every word in the examination question is important, and candidates should become proficient in formulating lists of major issues arising out of or suggested by the question stem. As examples see some of our thoughts below. Particularly candidates need to be able to talk about assessment (especially with regard to associated injuries and high risk features), immediate management priorities, and disposition considerations including "other" social (and often important) issues.
Being able to draw out these associations is a critical skill for candidates to develop in order to succeed in the fellowship examination.
1. A full assessment is needed.
We need to get a full history of how the injury occurred i.e.., what is the exact mechanism? We need to exclude other injuries, especially fractures of the orbit and globe rupture. Traumatic hyphaemas are usually the result of projectiles, however the abrasion may not fit in with this story. This is a grade 2 hyphaema ie., 1/3-1/2 of the pupil is obscured.
The history should include:
- past history
- medications as well as..
- immunisation status, as this is a potentially tetanus prone wound.
Examination should include:
- visual acuity as well as..
- CN III, IV, VI, for possible EOM entrapment, plus...
- an afferent pupillary defect and
- slit lamp examination.
Tonometry will also be needed as raised intraoccular pressure occurs in about 1/3 of cases. As a caveat if a globe rupture is suspected tonometry should not be performed as extra pressure may worsen extrusion of ocular contents. A globe rupture should be suspected with enopthalmos (intraoccqular content loss), exophthalmos due to retro-orbital haemorrhage, and a tear shaped or otherwise irregular pupil. Candidates should be prepared to mention the absence of these as important findings if required. Certainly the absence of an irregular pupil is an important negative finding in the photo above.
2. Most injuries require management
Management is a shield over the eye, rest, analgesia and sitting at a 30-45 degree angle to hasten clearing of the eye and improvement of visual acuity. An ophthalmologist should be quickly consulted by the emergency physician regarding this injury.
3. Disposition and social issues should always be considered.
Admission is indicated in this patient firstly because of the size of haematoma (certainly if there is any sickle cell trait) and secondly because there may be no-one available at home, which may be evidenced by the parents/carers not being present. Clued in candidates will also raise the issue as to why the parents are not present as the implication in the question is that this injury occurred earlier in the day (prior to school), and possibly represents non-accidental injury. Fellowship level candidates always do well to show perspective by consideration of NAI in paediatric presentations.